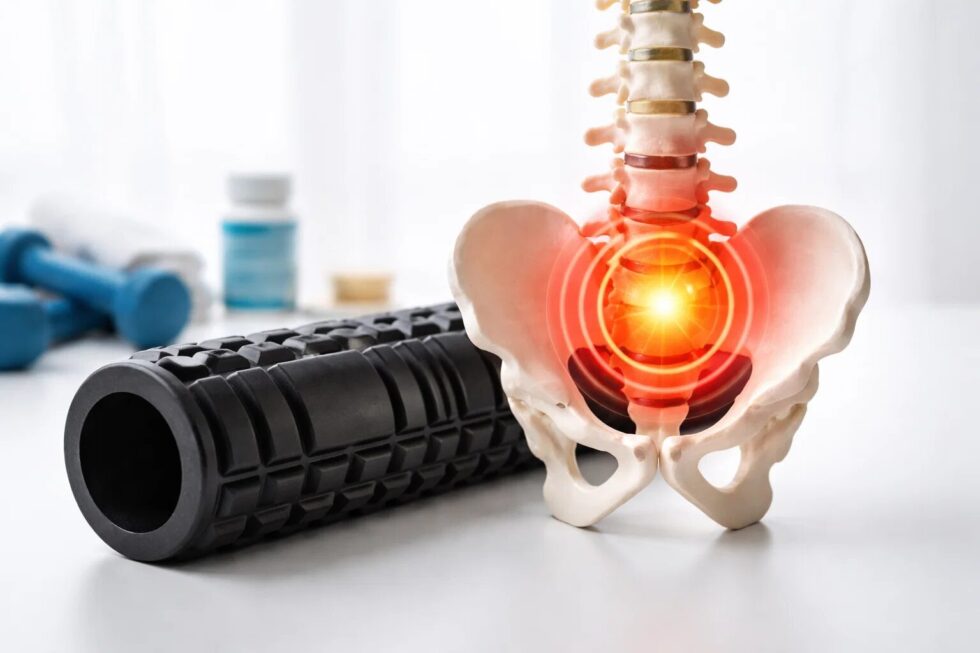
Sharp lower back pain often strikes like a lightning bolt during the most mundane movements of daily life. This sudden physical restriction leaves many people frozen in a painful, hunched position known as an antalgic posture. The body instinctively adopts this crooked stance to protect the spinal nerves from further perceived irritation or pressure. Muscles in the lumbar region undergo intense spasms that act as a natural but agonizing splint for the spine. Patients frequently describe the sensation as being locked or jammed in place without any warning or prior injury. Understanding the immediate steps for relief can prevent a short-term episode from turning into a chronic medical issue. Professional guidance is essential for navigating these frightening moments of total physical immobility and radiating nerve discomfort. Modern physiotherapy and conservative treatments offer effective ways to regain mobility and reduce the inflammation of soft tissues. As noted by the The WP Times, early intervention and proper movement patterns are key to recovering from acute lumbar episodes quickly.
Immediate steps for acute lumbar episodes
When the back locks up, the first priority is to find a position that unloads the spinal discs. Many specialists recommend the 90-90 position where you lie on the floor with legs resting on a chair. This posture flattens the lumbar curve and allows the overactive muscles to begin the process of gradual relaxation. Avoid total bed rest for more than two days as it can actually stiffen the joints further. Heat therapy can be beneficial for relaxing tight muscles, while cold packs help if there is active inflammation. Gentle breathing exercises help lower the body’s stress response, which often amplifies the perception of intense physical pain. It is important to monitor for "red flag" symptoms like numbness or loss of bladder control immediately. Walking short distances around the room is better than sitting on a soft sofa for long periods. The following list outlines practical items and actions that can assist during the first forty-eight hours of recovery.
- Find a firm surface to lie down on instead of a soft mattress
- Apply a heating pad for twenty minutes every few hours to soothe spasms
- Take over-the-counter anti-inflammatory medication if approved by your personal doctor or pharmacist
- Perform very slow pelvic tilts only if they do not increase the sharp pain
- Avoid lifting any objects, even light ones, until the initial muscle guarding subsides
- Use a small pillow between the knees when sleeping on your side for alignment
- Contact a physical therapist to schedule a diagnostic assessment as soon as possible
Maintaining a calm mindset is crucial because fear often leads to more muscle tension and restricted breathing patterns. Most cases of acute back locking are muscular or ligamentous in nature rather than permanent structural damage. Recovery usually follows a predictable path where the intensity of the pain decreases over several days of care. If the pain radiates down the leg, it might indicate irritation of the sciatic nerve requiring specific movements. Consistent movement, even if limited to a few steps, keeps the blood flowing to the damaged spinal tissues.
Understanding the causes of sudden back locking
The phenomenon of being unable to straighten up is usually caused by a combination of factors and triggers. Static loading from sitting at a desk for hours often weakens the core muscles responsible for spinal stability. A sudden twist or a heavy lift then acts as the final trigger for a protective muscle shutdown. In some cases, a small bulge in an intervertebral disc may touch a sensitive nerve root nearby. This causes the brain to send emergency signals to the back muscles to seize up and prevent movement. Dehydration and poor posture during the day also contribute to the vulnerability of the lower lumbar segments. Medical professionals categorize these events to determine if the cause is discogenic, muscular, or related to joint dysfunction. The data below shows common triggers and the typical recovery timelines associated with various types of back issues.
| Type of Issue | Primary Trigger | Typical Recovery Time | Recommended Initial Action |
| Muscle Strain | Sudden lifting | 1 to 2 weeks | Heat and gentle walking |
| Disc Irritation | Twisting while bending | 4 to 6 weeks | Nerve gliding and posture correction |
| Facet Syndrome | Sudden extension | 2 to 3 weeks | Manual therapy and core bracing |
| Ligament Sprain | Repetitive bending | 1 to 3 weeks | Compression and rest from triggers |
After the initial inflammatory phase passes, the focus must shift toward long-term prevention and strengthening of the core. Many people find that specific exercises targeting the transversus abdominis help prevent future episodes of getting stuck. Learning proper hip hinging techniques ensures that the spine stays neutral during heavy lifting or daily household chores. It is helpful to set reminders to stand up and stretch every thirty minutes during the working day. Investing in an ergonomic chair or a standing desk can significantly reduce the cumulative strain on the lower back. Strengthening the gluteal muscles also provides a stable base for the spine and reduces the load on lumbar joints.
Рsychological impact of sudden physical immobilization
Sharp lower back pain creates a significant psychological burden that often slows down the physical healing process. When the body suddenly locks, the brain enters a state of high alert known as hypervigilance. This mental state causes the nervous system to amplify pain signals as a protective mechanism. Many patients develop a fear of movement, which leads to secondary muscle stiffness and avoidant behavior. Breaking this cycle requires cognitive reassurance that most acute episodes do not indicate permanent structural failure. Breathing techniques and mindfulness can lower cortisol levels and reduce the overall perception of lumbar distress. Understanding the mind-body connection helps patients navigate the frustrating days of restricted mobility with more confidence. Positive mental framing is just as important as physical therapy for a full and lasting recovery.
- Practice diaphragmatic breathing to calm the overactive sympathetic nervous system
- Remind yourself that acute pain is usually a temporary protective response
- Set small daily goals for movement to rebuild confidence in your spine
- Avoid searching for catastrophic medical diagnoses online during the initial healing phase
- Consult with a specialist who explains the mechanical nature of your specific pain
- Focus on what you can still do rather than focusing on limitations
- Use relaxation recordings to help improve sleep quality during the first few nights
The recovery process is often non-linear, meaning some days may feel more restricted than others. Patients who remain calm and follow a structured movement plan tend to recover much faster. It is vital to recognize that the intensity of the sensation does not always equal the severity of the injury. Gradual exposure to normal activities helps the brain recalibrate its threat assessment of lumbar movements. Maintaining social connections and light hobbies can distract the mind from the localized physical discomfort. Professional support from a therapist can provide the necessary tools to manage the anxiety of future episodes.
Advanced diagnostic methods for recurring lumbar issues
When sharp lower back pain becomes a recurring event, modern diagnostics offer a deeper look into the underlying mechanics. Magnetic resonance imaging provides clear views of soft tissues, including intervertebral discs and the neural pathways. Electromyography can be used to assess the electrical activity of muscles and detect any nerve conduction delays. These tools allow clinicians to differentiate between simple muscle guarding and more complex conditions like stenosis. Early diagnostic clarity prevents the misuse of heavy medications or unnecessary invasive procedures for minor issues. Understanding the exact source of the irritation allows for a more targeted and effective rehabilitation program.
| Diagnostic Tool | Primary Focus | Use Case | Preparation Needed |
| MRI Scan | Soft tissue and discs | Suspected disc herniation | Removal of metal objects |
| X-Ray | Bone structure | Checking for fractures or slips | None |
| EMG Test | Nerve and muscle function | Radiating leg pain or weakness | No lotions on the skin |
| Physical Exam | Range of motion | Initial assessment of mobility | Comfortable clothing |
Detailed imaging is most useful when the physical symptoms do not improve after several weeks of conservative care. Most practitioners start with a thorough manual assessment before moving to expensive technological scans. Identifying specific movement triggers helps in creating a customized exercise protocol for the individual patient. Functional testing often reveals weaknesses in the kinetic chain that contribute to lumbar overload. Long-term success depends on addressing these global imbalances rather than just treating the localized pain site. Accurate data from these tests empowers the patient to take control of their spinal health journey.
Frequently Asked Questions
How long does the acute phase of sharp lower back pain typically last?
In 2026, clinical data suggests the most intense muscle guarding usually subsides within 48 to 72 hours. During this window, the body transition from an emergency inflammatory response to a gradual repair phase where movement becomes easier.
Should I use ice or heat when I experience sharp lower back pain?
Most specialists recommend using ice for the first 24 hours to reduce acute inflammation and numb the area. After the initial day, switching to heat therapy helps relax the protective muscle spasms and improves local blood circulation for healing.
Can I continue working if I have sharp lower back pain?
If your job involves heavy lifting or prolonged sitting, it is best to take a short break or modify your tasks. For office workers, using a standing desk and taking walking breaks every twenty minutes can prevent the spine from locking further.
What are the warning signs that sharp lower back pain is a medical emergency?
You must seek immediate medical attention if the pain is accompanied by a sudden loss of bowel or bladder control. Other red flags include significant leg weakness, numbness in the saddle area, or a fever that occurs alongside the back episode.
Is it safe to stretch during a sudden episode of sharp lower back pain?
Aggressive stretching should be avoided while the muscles are in a state of acute spasm as it may trigger more guarding. Stick to very gentle pelvic tilts or the "90-90" resting position until the sharpest sensations begin to fade after a few days.
Read about the life of Westminster and Pimlico district, London and the world. 24/7 news with fresh and useful updates on culture, business, technology and city life: Padel boom in Britain: what it is, who invented it and where to play in London in 2026